ICRMA offers statutory workers' compensation coverage to its members through a combination of self-insurance and excess insurance.
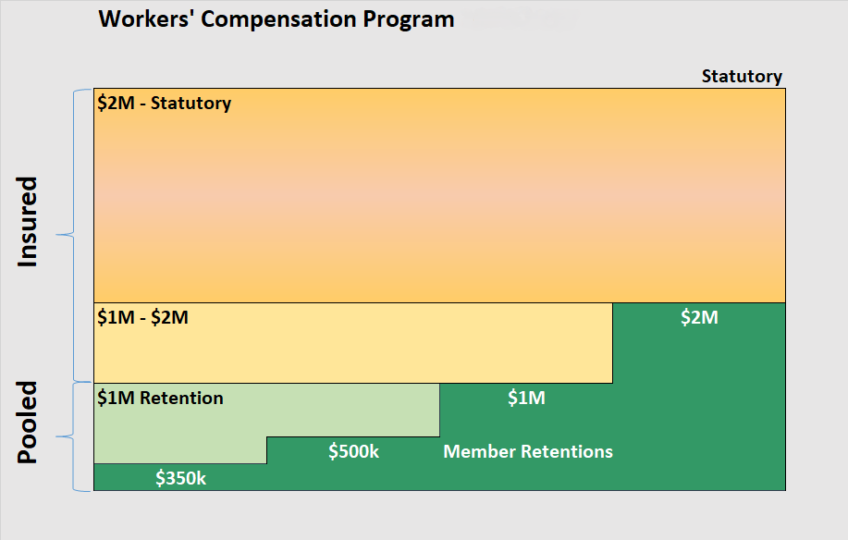
To accommodate different risk appetites, each public agency can determine the level of risk they are comfortable with. For the 2025-2026 program year, the ICRMA pooled retention is set at $1 million. The chart below illustrates how the various loss layers are funded from the members' retentions through the excess insurance.
ICRMA's Workers' Compensation Program Manager ensures effective claims management by providing oversight, conducting periodic claim file reviews, reporting losses to the excess carrier, and evaluating the performance of the program TPA.
Report a Workers’ Compensation Claim
Workers’ Compensation claims should be reported directly to ICRMA’s Third Party Claims Administrator (TPA), through their portal at http://www.adminsure.com.
The member's TPA will report excess claims to ICRMAwcprogram@adminsure.com.
For questions, please contact ICRMA’s Workers’ Compensation Program Manager, Kristen Vanscourt. The Program Manager will be responsible for communicating with excess insurer(s).
Third Party Administrators
ICRMA’s Governing Board has adopted performance standards for the Workers’ Compensation TPA to ensure appropriate claims handling.
Defense Panel
ICRMA’s Governing Board has adopted Litigation Management Policies and Procedures to ensure appropriate claims handling.
Workers’ Compensation Approved Defense Panel listing located in member-only section.
Nurse Triage
When an employee is injured, he/she is instructed by the member to call the Nurse Triage line provided by the TPA. A registered nurse completes a series of triage questions which will determine whether or not a medical referral to the city’s industrial clinic needs to be made. A copy of the report generated by the nurse is e-mailed to the city contact, ICRMA’s program manager, and to the TPA.
Cal/OSHA
Cal/OSHA recently confirmed that California employers must electronically report injury and illness data via federal OSHA Injury Tracking Application (ITA) online portal. Please reference:
https://www.dir.ca.gov/dosh/calosha-updates/log300-reporting.html
https://www.osha.gov/news/newsreleases/trade/04302018
Federal OSHA Injury Tracking online portal: https://www.osha.gov/injuryreporting/index.html. This link provides all the details regarding this employer requirement. Reference ITA Job Aids.